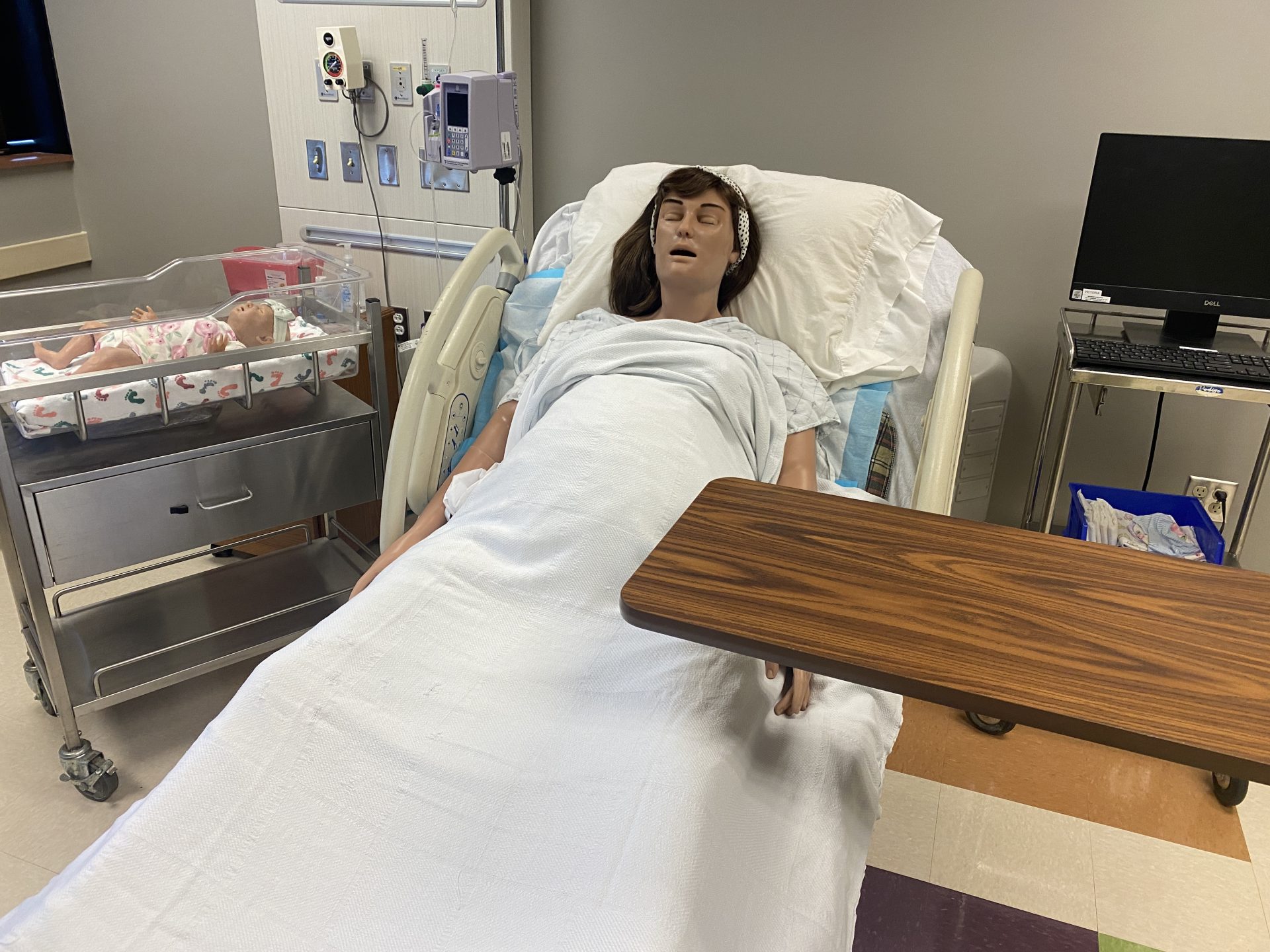
Victoria is a labor and delivery manikin at the University of Oklahoma's Fran and Earl Ziegler College of Nursing. The computerized dummy allows students to practice their skills.


Victoria is a labor and delivery manikin at the University of Oklahoma's Fran and Earl Ziegler College of Nursing. The computerized dummy allows students to practice their skills.
A group of OU nursing students is practicing their hemovac skills. Those are little contraptions that health workers can use to drain fluid buildup after a surgery. These ones are filled with water dyed to look like blood.
The drains are sitting on tables in a room that mimics a hospital wing. There are hospital beds, monitors, a linens shelf, everything. Even patients. Granted, the patients are not people but very high-tech manekins.
They’re in a building in Research Park — a complex in Oklahoma City’s biomedical district. It used to house a call center. But last spring, OU president Joseph Harroz Jr. announced the university would be expanding its nursing program.

One of the many practice areas in the OU College of Nursing’s training spaces.
Several other schools are pitching in, too. Rogers State University ramped up its number of slots. Oklahoma State University just announced it created a bachelor’s of nursing program.
This is all in an effort to curtail Oklahoma’s decades-long nursing shortage. The state ranks 46th in the nation for nurses per capita, and of course, the pandemic has only made that worse.
But all along, one of the major contributing factors to that shortage has been nursing school. There are a finite number of slots offered, and Oklahoma hasn’t had enough. Why? It’s complicated.
For one, nursing programs are different from something like history or liberal arts. Dr. Julie Hoff is the dean at OU’s nursing school. She says these students sit in lectures like everyone else, but they have skills labs, like that hemovac one. Nurses have to actually work in hospitals and other treatment centers. They have to build up enough supervised hours and experience to graduate and qualify for their boards. Like everything else in health care, that got harder during the pandemic.
“The bottleneck, it’s clinical,” Hoff said. “During COVID, the concern was, can we really take the risk of sending a student into the clinical setting? … Post-COVID nurses are, you know, nurses are tired, they’re stressed. Staffing is challenging.”
While all of this was happening, simulation equipment continued to evolve and improve. And several schools, including OU, got grants and donations that let them invest in that technology.
These simulations don’t look like computer games. Victoria, a labor and delivery manikin, gives students experience delivering babies. Among other things, she can yell in pain and say she needs an epidural.
Students get to test their skills using these computerized dummies. And unlike in a real clinical setting, they’re the nurse in charge. They can practice undergoing the stress of managing major complications, like a sudden hemorrhage. Victoria will gush fake blood to simulate that.
This technology has been a boon for Rogers State University too, says Dr. Carla Lynch, the nursing department head. That school is partnering with Saint Francis to add more slots. Soon, it will turn out 32 more graduates per year.
“The Cherokee Nation has donated money and allowed us to expand our simulation capabilities,” she said. “And the Oklahoma Board of Nursing has allowed us to use … simulated patient care experiences to substitute for up to 30% of clinical time.”
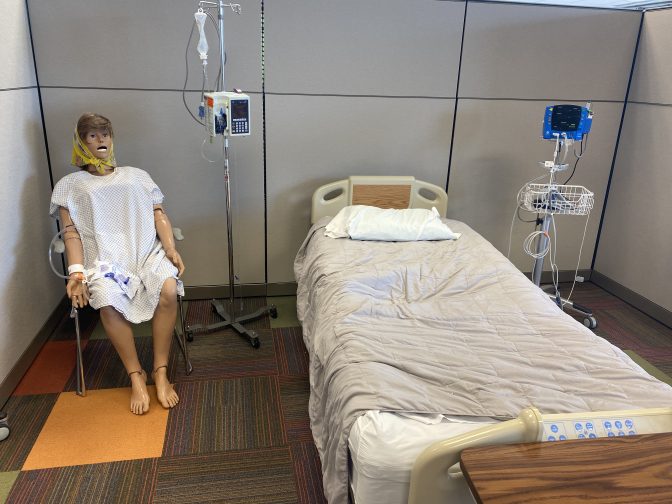
The OU College of Nursing has invested millions of dollars into simulation technology, such as this manikin. These computerized dummies can talk with students and simulate medical problems like hemorrhages.
As helpful as these investments in simulation have been, they’re not a sole fix.
“The two main liberty limiting factors for expansion of nursing programs is clinical space off site like we talked about and the nursing faculty. Most of our graduates make more than we do as faculty members — when they graduate. And not only that, we require nursing faculty have to go back and get a master’s or doctorate degree, which cost additional money, additional time and energy to make less money, you know.”
Hoff, over at OU, says although the nursing shortage is a major problem in Oklahoma, it can seem invisible from the outside.
“The nursing crisis is all of our problem,” she said. “But you don’t realize it until you’re trying to access care.”
She says one resource critical to curtail the shortage is public support for the field.