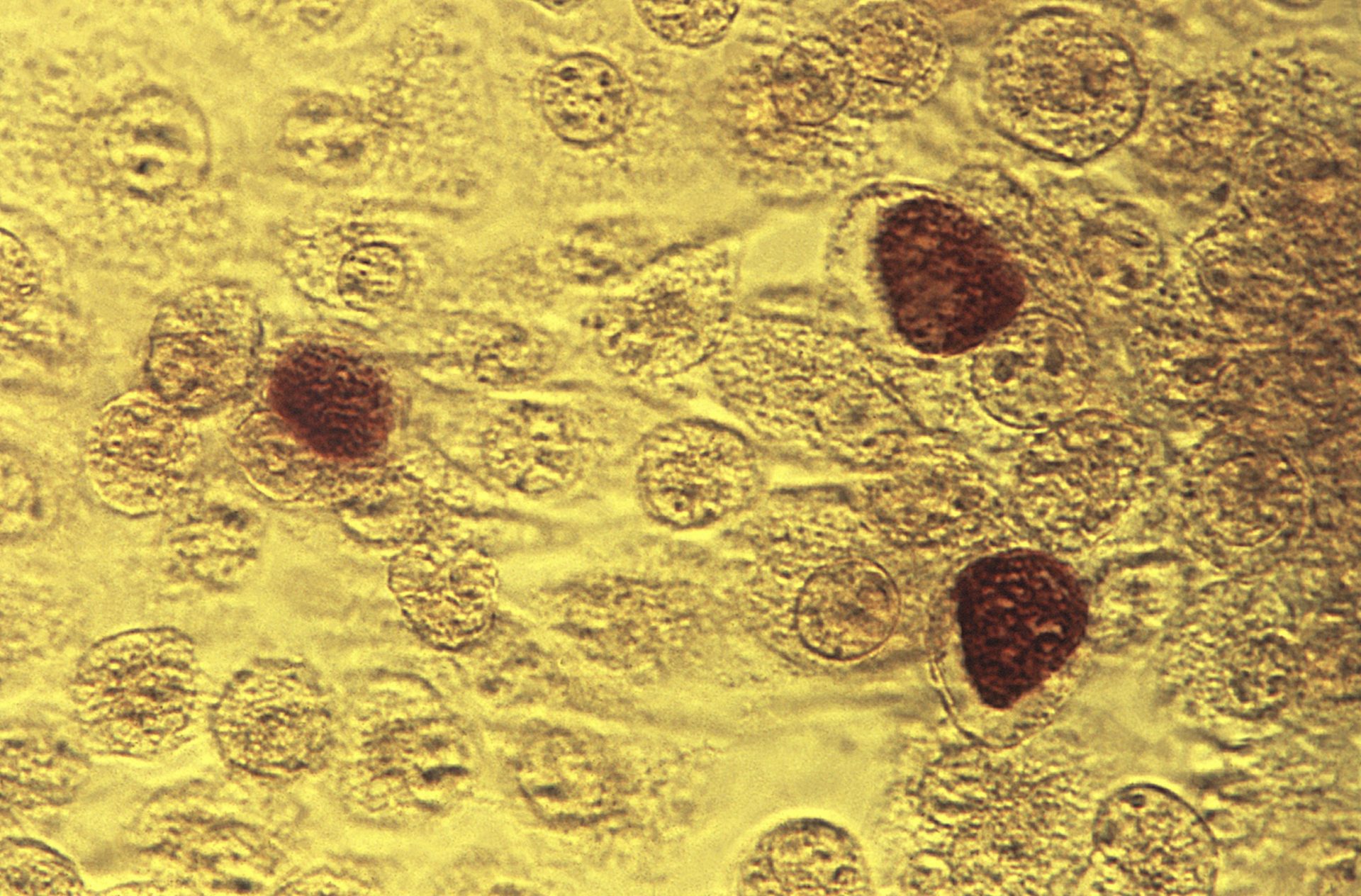
AP FILE - This 1975 microscope file image made available by the the Centers for Disease Control and Prevention shows Chlamydia trachomatis bacteria magnified 200X. (Dr. E. Arum, Dr. N. Jacobs/CDC)


AP FILE - This 1975 microscope file image made available by the the Centers for Disease Control and Prevention shows Chlamydia trachomatis bacteria magnified 200X. (Dr. E. Arum, Dr. N. Jacobs/CDC)
The newest round of CDC numbers sound bad. No. 11 for chlamydia. No. 5 for gonorrhea. No. 4 for syphilis. But they aren’t too surprising to Terrainia Harris.
“Of course, we’re seeing this on kind of a daily basis, so we can automatically see that we’re getting an increase because we literally see more cases coming in,” she said.
Harris is the administrative program manager for the state’s Sexual Health and Harm Reduction Service. And she is one of several health officials saying these high rates — revealed in the CDC’s STI data for 2020 — aren’t new for Oklahoma.
They believe the pandemic worsened STI rates in much the same way that it worsened other health outcomes. It stymied access to care — by creating barriers for patients who need it and for health workers who provide it.
Ronneal Mathews is the director of community engagement for Thrive OKC, a nonprofit organization that advocates for access to reproductive health.
“I think we’re seeing a lot of the fallout from the COVID-19 pandemic, really,” she said. “We’re looking at people who had a reduced frequency of in-person health care services and routine visits and screenings.”
During the height of the pandemic some people opted out of screenings. They were simply nervous about going into health facilities.
Ellen Niemitalois the clinical services director for Tulsa Health Department. She says when it comes to STIs, those screenings are critical. Many of the infections either take months to show symptoms or never do. In the case of syphilis, symptoms can show up, then appear to resolve, even though the virus is still alive and kicking.
“Chlamydia is probably the most easily transmitted without any symptoms because 75-to-85 percent of all people who have the infection are asymptomatic,” she said.
Mathews points out that people who still seek care face obstacles, too. Early on in the pandemic providers leaned heavily on telemedicine. Labs had supply and labor shortages, problems felt across most industries.
“People had a lot of lapses in health insurance coverage due to, you know, employment losses and things like that during the pandemic,” Mathews said.
So all of those issues likely worsened the trends, but Oklahoma was already trending high. Harris says on the state level, one infection in particular has been surging.
“The congenital syphilis rates have been going up — pretty astronomically — for the last several years,” she said. “Since 2017, there’s actually been a six hundred and fifty seven percent increase in congenital syphilis cases.”
Tulsa has seen a surge too. Niemitalo says that’s especially concerning for infants born with syphilis.
“Cases of congenital syphilis, if untreated, can lead to some very poor outcomes, whether it be fetal death or miscarriage, or some disabilities and congenital malformations in the baby, premature birth,” she said. “So really, it can be very serious, which is so tragic because it’s treatable.”
If untreated in adults, the virus can cause damage to the brain, to vision and to several organs.
So where do we go from here? The main thing each of these experts came back to time and again was encouraging testing. They say public health workers and others need to help get information and resources to the people who need it.
Harris says they are also working to address stigma, which can affect patients — but providers too. For example, she says there’s a common story for patients who come in with symptoms and a ring on their finger.
“They ask to be tested for one of the infections, and the physician or nurse or nurse practitioner would tell them, ‘Well, you’re married, you don’t need to worry about that,’ or, ‘You’re not in that population. So there’s still this kind of stigma of a difference between those people that get infections and those that don’t.”
Mathews notes these figures need context. Sexual health is a part of overall health. High rates of infection don’t happen in a vacuum.
“It’s the symptom of a bigger issue,” she said.
The STI numbers aren’t likely to improve as long as Oklahoma remains in the bottom five for overall health outcomes and continues to experience widespread barriers to medical access.